Stuck in Silos? How AI Workflow Automation Is Breaking Barriers in Healthcare Organizations

The healthcare industry has long been at the cutting edge of innovation when it comes to clinical technologies—robotic surgeries, advanced imaging, precision medicine. But behind the scenes, many healthcare organizations still grapple with outdated, siloed systems that slow down operations, fragment patient care, and increase costs.
Siloed data and disconnected workflows across departments like administration, supply chain, finance, labs, and patient services are more than just an inconvenience—they’re one of the biggest threats to healthcare efficiency and patient outcomes. As demands for speed, compliance, and patient-centricity intensify, organizations can no longer afford to let silos hold them back.
Enter AI-powered workflow automation, a transformative force enabling hospitals, clinics, and healthcare networks to break down barriers, unify processes, and deliver smarter, more agile care operations.
Data Silo:
An isolated repository of data controlled by one department or system that is not accessible or shared with other departments or systems. In healthcare, data silos between clinical, administrative, pharmacy, radiology, and lab systems result in fragmented patient records, duplicated data entry, and incomplete information at the point of care.
Interoperability:
The ability of different healthcare information systems, devices, and software to communicate, exchange, and use patient data seamlessly. HL7 FHIR (Fast Healthcare Interoperability Resources) is the current US federal standard for healthcare data exchange, required by the 21st Century Cures Act for EHR vendors.
HL7 FHIR:
Fast Healthcare Interoperability Resources — the modern RESTful API standard for healthcare data exchange. FHIR enables different healthcare applications (EHRs, lab systems, patient apps, AI tools) to exchange structured clinical data using standard resource formats (Patient, Observation, Encounter, Medication, etc.) over secure HTTP APIs.
Care Coordination:
The deliberate organization of patient care activities and information sharing among all participants concerned with a patient’s care to achieve safer and more effective care. AI improves care coordination by automating information routing, alerting care team members to care gaps, and ensuring the right information reaches the right provider at the right time.
In this blog, we’ll explore how AI automation platforms are reshaping healthcare by integrating systems, orchestrating workflows, and unlocking collaboration across the enterprise.
The Hidden Cost of Silos in Healthcare
Disconnected systems and siloed processes create a ripple effect of inefficiency across healthcare operations:
-
- Fragmented Data: Patient information often lives across multiple systems—EHR (Electronic Health Records), ERP (Enterprise Resource Planning), CRM (Customer Relationship Management), and LIMS (Laboratory Information Management Systems)—making it difficult to form a single view of patient journeys or organizational performance.
- Manual Handoffs: Teams waste countless hours emailing spreadsheets, calling colleagues, or re-entering data into multiple platforms, leading to errors and duplication.
- Delayed Decisions: Without real-time insights, managers struggle to allocate resources, forecast demand, or respond quickly to operational challenges.
- Poor Collaboration: Clinicians, administrators, and support staff often work in parallel rather than in sync, reducing coordination and slowing down care delivery.
- Compliance Risks: Lack of integration increases the risk of inconsistent reporting and gaps in regulatory compliance, exposing organizations to fines and reputational damage.
The result? Slower service delivery, higher costs, staff burnout, and diminished patient satisfaction.
How AI Workflow Automation Breaks Barriers
Modern AI automation platforms don’t just digitize tasks—they orchestrate and optimize end-to-end healthcare workflows. By connecting disparate systems and applying machine learning intelligence, they empower organizations to streamline operations and improve outcomes.
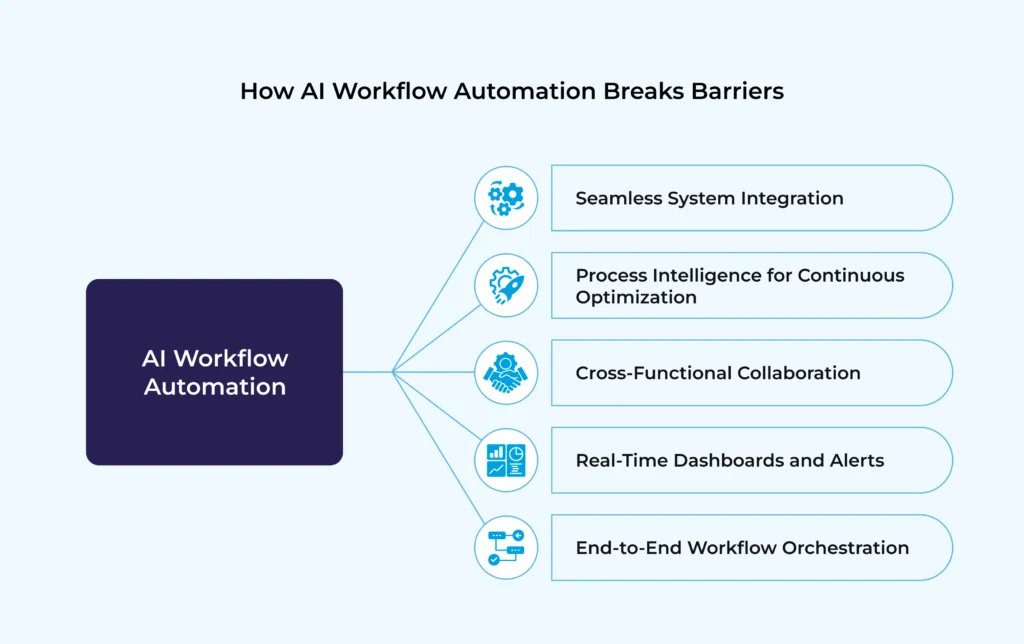 Here’s how AI workflow automation is breaking down silos in healthcare:
Here’s how AI workflow automation is breaking down silos in healthcare:
-
- Seamless System Integration
AI-powered automation platforms act as a bridge between critical systems like ERP, CRM, EHR, and LIMS. By connecting these traditionally siloed applications, healthcare providers gain unified visibility across the enterprise. For example: An automated workflow can integrate patient intake data from a CRM with scheduling in the EHR and billing in ERP, eliminating redundant data entry and ensuring accuracy across systems. - Process Intelligence for Continuous Optimization
Beyond simple automation, AI applies process intelligence—analyzing workflow patterns, detecting bottlenecks, and recommending improvements. Imagine a lab that struggles with delays in test result processing. AI can pinpoint where bottlenecks occur (e.g., manual data transfer from LIMS to EHR) and suggest automation to cut turnaround times dramatically. - Cross-Functional Collaboration
AI automation reduces the need for manual coordination between departments. Instead, digital workflows orchestrate tasks across teams, ensuring everyone has the right information at the right time. For instance, when a patient’s surgery is scheduled, automated workflows can simultaneously trigger:- Procurement to prepare necessary supplies,
- Finance to initiate pre-authorization,
- HR to schedule staff shifts, and
- Patient services to send reminders and instructions.
- This creates seamless collaboration without endless back-and-forth emails or phone calls.
- Real-Time Dashboards and Alerts
AI-enabled dashboards aggregate data across functions, providing decision-makers with real-time visibility into KPIs like patient throughput, staffing utilization, and supply chain performance. Automated alerts notify teams about issues – such as delayed lab results or low stock of critical supplies – allowing immediate corrective action. - End-to-End Workflow Orchestration
AI doesn’t just optimize isolated tasks—it orchestrates workflows across entire healthcare journeys. From patient admission to discharge, automation ensures that processes flow smoothly, handoffs are seamless, and compliance is built in.
- Seamless System Integration
This holistic approach reduces errors, shortens cycle times, and improves patient satisfaction.
Business and Clinical Benefits of AI Automation
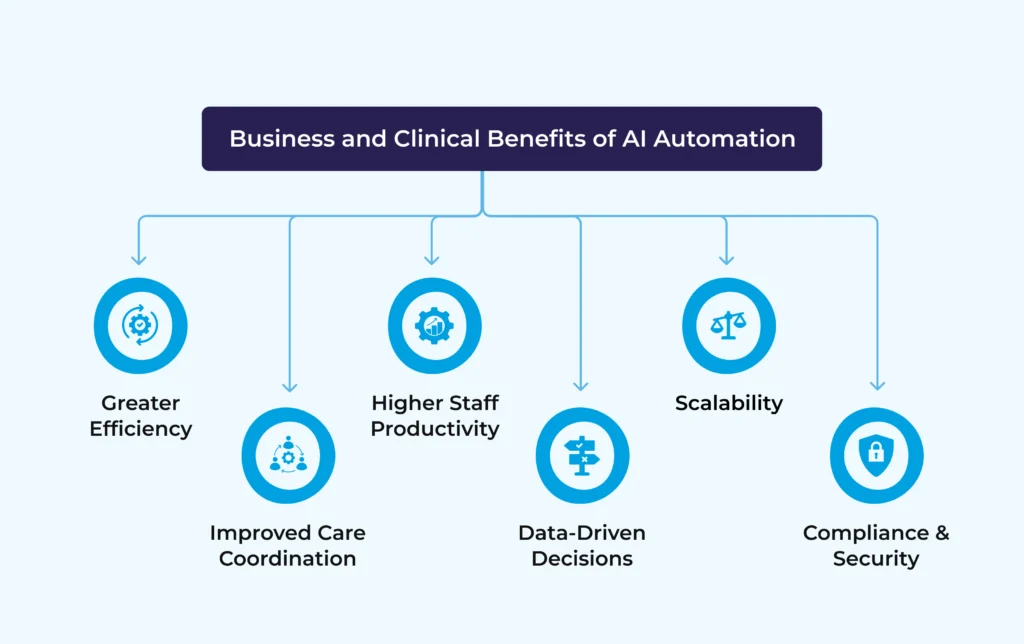 The shift from siloed operations to AI-driven workflows delivers both operational and clinical benefits:
The shift from siloed operations to AI-driven workflows delivers both operational and clinical benefits:
-
- Greater Efficiency: Automated processes cut redundant tasks and reduce manual workload.
- Improved Care Coordination: Cross-departmental workflows create a more unified patient experience.
- Higher Staff Productivity: Clinicians and administrators can focus on value-added activities instead of routine tasks.
- Data-Driven Decisions: Unified, real-time insights allow leaders to make faster, more informed choices.
- Scalability: AI workflows can easily adapt to growing patient volumes or evolving service demands.
- Compliance & Security: Automated data handling reduces human error and supports audit trails, ensuring regulatory adherence.
Real-World Use Cases
To bring this to life, here are a few examples of how healthcare organizations are using AI workflow automation:
-
- Patient Intake & Scheduling: Automating intake forms and connecting them directly to EHRs and scheduling systems reduces wait times and paperwork.
- Lab-to-Physician Reporting: AI workflows ensure lab results are automatically routed to the right physicians and uploaded into EHRs with alerts for abnormal values.
- Claims & Billing: Automation speeds up claim submissions, checks for errors, and ensures timely reimbursement.
- Supply Chain Management: Predictive AI models forecast supply needs and automate reordering to prevent stockouts of critical equipment.
- Staffing Optimization: AI recommends staffing schedules based on patient load predictions, reducing overtime and burnout.
Building a Smarter, Connected Future
The healthcare industry is under constant pressure to do more with less—deliver better care, faster, at lower cost, while meeting strict compliance standards. Breaking free from siloed systems and processes is no longer optional; it’s mission-critical.
By embracing AI workflow automation, healthcare organizations can create a truly connected ecosystem where data flows freely, teams collaborate effortlessly, and operations run smarter. This not only drives business efficiency but also translates directly into better patient care and outcomes.
Conclusion
Healthcare silos have held organizations back for decades, but AI automation is rewriting the rules. By integrating systems, orchestrating workflows, and enabling real-time visibility, AI is transforming how healthcare providers operate.
 The result? Greater agility, fewer errors, improved compliance, and a patient experience that truly matches the promises of modern healthcare.
The result? Greater agility, fewer errors, improved compliance, and a patient experience that truly matches the promises of modern healthcare.
The future belongs to healthcare organizations that move beyond silos and embrace connected, intelligent workflows powered by AI.
Key Takeaway
-
- Healthcare data silos are the primary barrier to AI effectiveness — AI is only as good as the data it can access.
- HL7 FHIR interoperability is the technical foundation that enables AI to break down silos between clinical systems.
- RPA (Robotic Process Automation) bridges legacy systems that lack modern APIs — automating data entry between non-integrated systems.
- Care coordination automation reduces preventable adverse events by ensuring all care team members have current, complete patient information.
- The ROI of healthcare workflow automation is highest in processes that currently involve the most manual data re-entry across systems.
- Successful healthcare AI integration requires clinical champion involvement — IT-only implementations fail at the adoption stage.







